Kirksville (660) 665-9000
May 2024
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
A Rare Genetic Disease and Its Link to Foot Stress Fractures
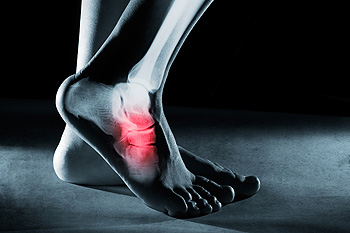
Hypophosphatasia, or HPP, is a rare genetic disorder characterized by impaired bone mineralization, leading to skeletal abnormalities and increased susceptibility to fractures. While HPP primarily affects bones throughout the body, including the legs and spine, it can also manifest in the feet, causing a range of complications, including stress fractures. In individuals with HPP, the deficiency of alkaline phosphatase enzyme disrupts the normal bone mineralization process, resulting in weakened bones that are prone to fracture under stress or pressure. Foot stress fractures, particularly in the metatarsal bones or heel, can occur due to repetitive impact or weight-bearing activities, exacerbating the existing skeletal fragility associated with HPP. Recognizing the potential connection between HPP and foot stress fractures is critical for an accurate diagnosis and appropriate management strategies. Early intervention, including wearing supportive footwear, orthotic devices, and lifestyle modifications, can help mitigate the risk of fractures and improve the quality of life for individuals living with this rare genetic disease. If you believe you have a foot stress fracture, it is strongly suggested that you consult a podiatrist who can successfully treat these breaks, and determine if HPP is a contributing factor.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact Deborah Holte, DPM from Northeast Missouri Foot Clinic. Our doctor can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our office located in Kirksville, MO . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Biomechanics in Podiatry
Podiatry is a branch of medicine that deals with the study, diagnosis, and treatment of foot and ankle conditions. There are various subdivisions in podiatry; biomechanics is one of them. Biomechanics is the way in which the bones, muscles, and joints of the feet and lower limb interact with each other.
Our feet play crucial roles in the way we move, and it is rare to have feet that are completely symmetrical. Common biomechanical issues include high or low arches or uneven leg heights. Excessive pronation often leads to fallen arches, or flat feet, and is a common cause of running injuries. People whose feet are over-pronated tend to have flexible and unstable feet. Pain is usually experienced during walking and running.
At times, people may be able to adapt to these abnormalities without any difficulties, but in other cases, these issues can cause a great deal of pain. This pain occurs because the joints, muscles, ligaments, and tendons are put under an excess amount of stress during movement. Common symptoms of biomechanical problems stemming from the feet include hip pain, knee pain, leg cramps, ankle pain, lower back pain, weak ankles, tripping, heel pain, Achilles pain, and shin splints.
Many biomechanical issues can be treated with orthotics. Orthotics are shoe insoles that are used to help control the way the foot operates. They can provide relief from foot pain, heel pain, and knee pain. Depending on your specific case, you may need to purchase over-the-counter orthotics or custom orthotics to fit your feet. Your podiatrist will be able to prescribe the perfect orthotic for your feet to help you walk around with ease.
Gait is defined as the way we move our bodies from one point to another. This is usually done by either walking or running. Gait analysis is a method used to assess the way we walk or run to highlight biomechanical abnormalities. Gait analyses are a great way to take a detailed look at how you walk and how your foot moves while you walk. An examination of the feet will help your podiatrist understand why you are suffering pain in other parts of your body.
Treating Symptoms of Foot Drop

Managing the symptoms of foot drop requires a multifaceted approach aimed at addressing its underlying causes while enhancing stability and mobility. The main symptom of foot drop is difficulty lifting the front part of the foot when you take a step. It can stem from muscular weakness, nerve damage in the leg, or injuries to the brain or spinal cord. Treatment with the help of a podiatrist focuses on strengthening the foot, ankle, and lower leg muscles to improve function and compensate for the lack of dorsiflexion. Wearing an ankle-foot orthosis can also provide support by maintaining proper alignment during walking, which reduces the risk of tripping and falling. Electrical nerve stimulation offers another avenue for improvement, facilitating muscle activation and enhancing walking ability in some cases. For severe or long-term foot drop caused by muscle paralysis, surgical intervention may be necessary to restore movement. Home modifications, such as removing clutter and using non-slip rugs, play a vital role in fall prevention. If you are experiencing symptoms of foot drop, it is suggested that you schedule an appointment with a podiatrist to explore appropriate treatment options.
If you have any concerns about your feet, contact Deborah Holte, DPM from Northeast Missouri Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Kirksville, MO . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Stretches for Plantar Fasciitis

If you have ever experienced the sharp, stabbing pain of plantar fasciitis, you know how debilitating it can be. Plantar fasciitis, caused by inflammation of the ligament running from the toes to the heel, often results from overuse. However, relief may be closer than you think and involves simple exercises. Begin by sitting with feet flat on the floor, lifting the leg with the sore foot, and placing that ankle on the opposite leg. Flex your toes toward your shin, feeling the stretch under your foot for five seconds, and repeat 10 times. Then, sit with your feet flat and place a frozen water bottle on the floor, rolling it under your foot for one to two minutes, focusing on painful areas. Similarly, use a golf or tennis ball to massage the sole of your foot, targeting painful areas. These simple stretches can provide immense relief, but for a more comprehensive treatment plan tailored to your specific needs, a podiatrist can help. This foot and ankle specialist can offer personalized advice and other methods to address plantar fasciitis effectively. For relief from plantar fasciitis pain, it is suggested that you consult a podiatrist today.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Deborah Holte, DPM from Northeast Missouri Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Kirksville, MO . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Blisters
Blisters are pockets of fluid that occur under the top layer of your skin. These fluid pockets are usually filled with pus, blood, or serum. Blisters may itch or hurt and can appear as a single bubble or in clusters.
The most common types of blisters are friction blisters. This type of blister may be caused by wearing shoes that are too tight. Friction blisters can also occur on the hands. A change in temperature may also cause blisters on the feet. In the freezing air, frostbite on your toes can lead to blisters, as well as sunburn from hot weather.
The best way to treat a blister is to keep it clean and dry. Most blisters will get better on their own. Once the skin absorbs the fluid within the blister, it will flatten and eventually peel off. You should avoid popping your blister unless you podiatrist does it for you. Additional treatment options include applying an ice pack to the blister or using over-the-counter blister bandages to cover the affected area.
If your blister becomes discolored, inflamed, or worsens it is advised that you speak to your podiatrist. Blisters that are yellow, green, or purple may be infected and require immediate medical attention. Blisters that are abnormally colored may be a sign of a more serious underlying health condition such as herpes.
Dealing with Blisters Between the Toes

Blisters between the toes can be a real pain, whether they're caused by friction, insect bites, burns, or infections. These little pockets of fluid can make each step a challenge. Friction is often the main cause of blisters between the toes. When your toes rub against each other or your shoes, the skin becomes irritated and leads to blister formation. Other causes of blisters between the toes include insect bites, burns, and various infections. While most blisters will heal on their own within a week or two, it's essential to resist the urge to pop them. Breaking a blister can increase the risk of infection and prolong the healing process. Instead, keep the blister clean and covered with a bandage. If the blister is particularly painful or shows signs of infection, it's best to seek medical attention from a podiatrist. Preventing blisters between the toes starts with wearing properly fitting shoes and socks. Avoid walking long distances in new shoes, and be sure to change socks if they become damp. If you have persistent or severe blisters between the toes, it is suggested that you seek help from a podiatrist for relief.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Deborah Holte, DPM of Northeast Missouri Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our office located in Kirksville, MO . We offer the newest diagnostic and treatment technologies for all your foot care needs.





